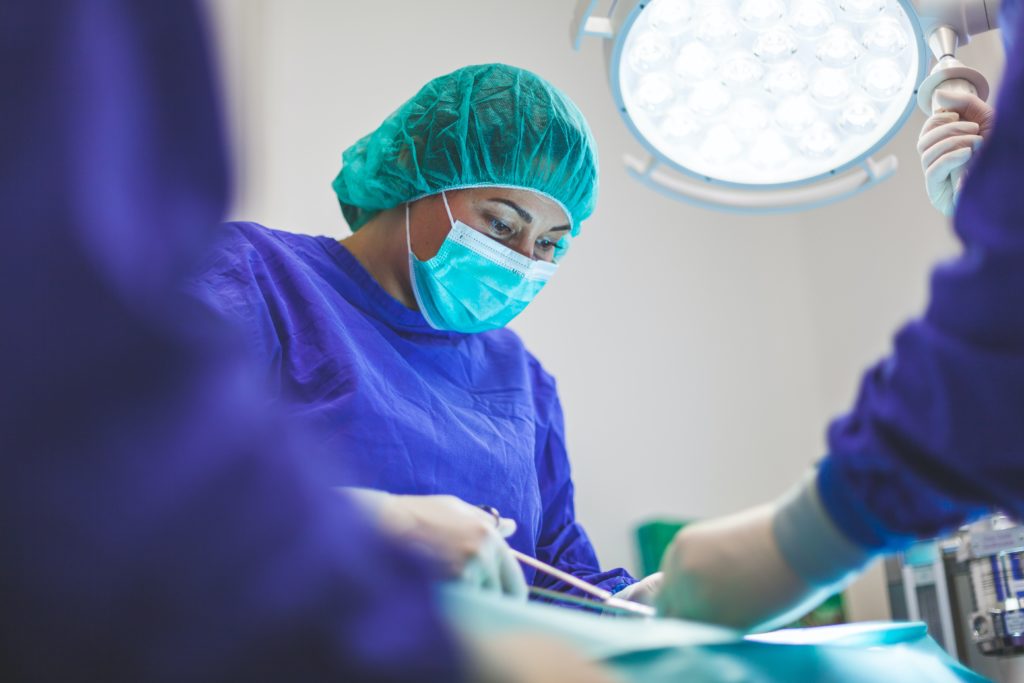
 During COVID-19, many surgeries were postponed or canceled for safety reasons. But sometimes people avoid surgery out of fear or anxiety. They worry about possible complications, pain, loss of mobility or productivity, and medication interactions afterward. At Pacific Surgical Center, doctors use the latest techniques and minimally invasive outpatient procedures to reduce downtime and the need for a long recovery. Within the outpatient surgery community, new techniques and trends help keep patients relaxed and stress-free.
During COVID-19, many surgeries were postponed or canceled for safety reasons. But sometimes people avoid surgery out of fear or anxiety. They worry about possible complications, pain, loss of mobility or productivity, and medication interactions afterward. At Pacific Surgical Center, doctors use the latest techniques and minimally invasive outpatient procedures to reduce downtime and the need for a long recovery. Within the outpatient surgery community, new techniques and trends help keep patients relaxed and stress-free.
Experts explain that “Pain is a dynamic and ever-changing phenomenon that requires multiple providers working closely together to best serve the patient. Leaders of pain management programs must regularly communicate with the patient’s referring provider, who is usually the primary care doctor…[but] there’s still a common misconception that chronic pain management often involves the use of opioids.”
These same experts acknowledge that “Patients decide to have their knees, hips, and shoulders replaced when the debilitating effects of degenerative joint disease impact their daily lives, preventing them from performing even the most basic tasks. The procedures pay off in the long run, but patients must endure significant pain during the early days of recovery before realizing the life-changing benefits.”
Preoperative education has been shown to be a tremendous comfort. Having time to sit down and discuss the procedure, have questions answered and worries addressed, and establish a relationship with your care team ahead of time is a critical piece of your post-surgery healing.
For those nervous about narcotics, know that the outpatient surgery industry is working hard to find ways of managing pain without relying on pills. Experts understand that “the stakes have never been higher. The national opioid overdose crisis has only worsened during the pandemic, creating a sense of urgency among physicians to find alternative ways to help their patients rest easy after surgery without exposing them to powerful painkillers that could lead to overuse or addiction.”
Beyond addiction, opioids have been linked to “respiratory depression, nausea, vomiting, constipation and altered mental status, which can complicate recovery or prolong inpatient admission.” In a recent study of patients undergoing ACL repair, half were treated with opioids and the other with “anti-inflammatories, acetaminophen and muscle relaxers…Pain scores in the non-opioid group were equivalent to those in the opioid group, and there were no significant differences in side effects among the patients.”
As always, education and a patient/doctor partnership are key. These non-opioid patients worked with a carefully timed pain-management schedule to best succeed. And, as always, don’t forget the “importance of involving all members of a patient’s care team—primary care physician, surgeon, anesthesiologist, pain specialist—in creating a pain management plan for the perioperative period as well as contingency plans for emergent needs. These coordinated efforts often eliminate worry and frustration for both patients and providers.”
There are even little easy, inexpensive, calming ways to help with surgical anxiety. You might even have them at home already. A California hospital provided one nervous patient “a plastic inhaler about the size of a lipstick container filled with calming lavender oil” and reported that “The patient used the inhaler frequently, almost like a calming blanket.”
Doctors explain that “studies have shown that between 60% to 90% of patients can experience pre-op anxiety and that it can be particularly prevalent in female patients. Furthermore, many patients cite the anxiety as the worst part of their overall surgical experience and the stress can in some cases be linked to poor post-op physiological outcomes.”
Because of this “aromatherapy is so valuable. It’s inexpensive, safe, and effective for many.” A nurse from Pennsylvania agrees. “Anytime we can avoid using medication and steer clear of its potential side effects, we try to do it. Medications should be used when necessary, and complements such as aromatherapy should coexist with them.”
Studies show that “anxiety seems to play a role in whether people suffer chronic pain after surgery.” Working with your care team to answer questions, explain the process and recovery journey, and iron out financial wrinkles beforehand means you can relax and recover in peace. At Pacific Surgical Center, their staff wants you back on your feet and ready to face the world like your old active, pain-free self. They’ll walk with you every step of the way and that definitely keeps stress and worry at bay.


